Gum disease — also called periodontal disease — is one of the most common chronic conditions in the United States, yet most patients don't know they have it until significant damage has already occurred. Unlike a cavity, which usually hurts, gum disease is largely painless in its early and middle stages. By the time it becomes uncomfortable, irreversible bone loss is often already underway.
The good news: caught early, gum disease is very treatable. The challenge is knowing what to look for. Here are five warning signs that should prompt a visit to a periodontist — not just your general dentist.
1. Bleeding When You Brush or Floss
This is the most common early sign, and the most commonly dismissed. Many patients assume bleeding gums are normal, or that they're brushing "too hard." They are not normal. Healthy gums do not bleed.
Bleeding is your body's inflammatory response to bacteria that have taken up residence at or below the gumline. The gum tissue becomes swollen, fragile, and prone to bleeding with even gentle contact. This stage is called gingivitis — and it is fully reversible with proper treatment. Ignored, it progresses to periodontitis, which is not.
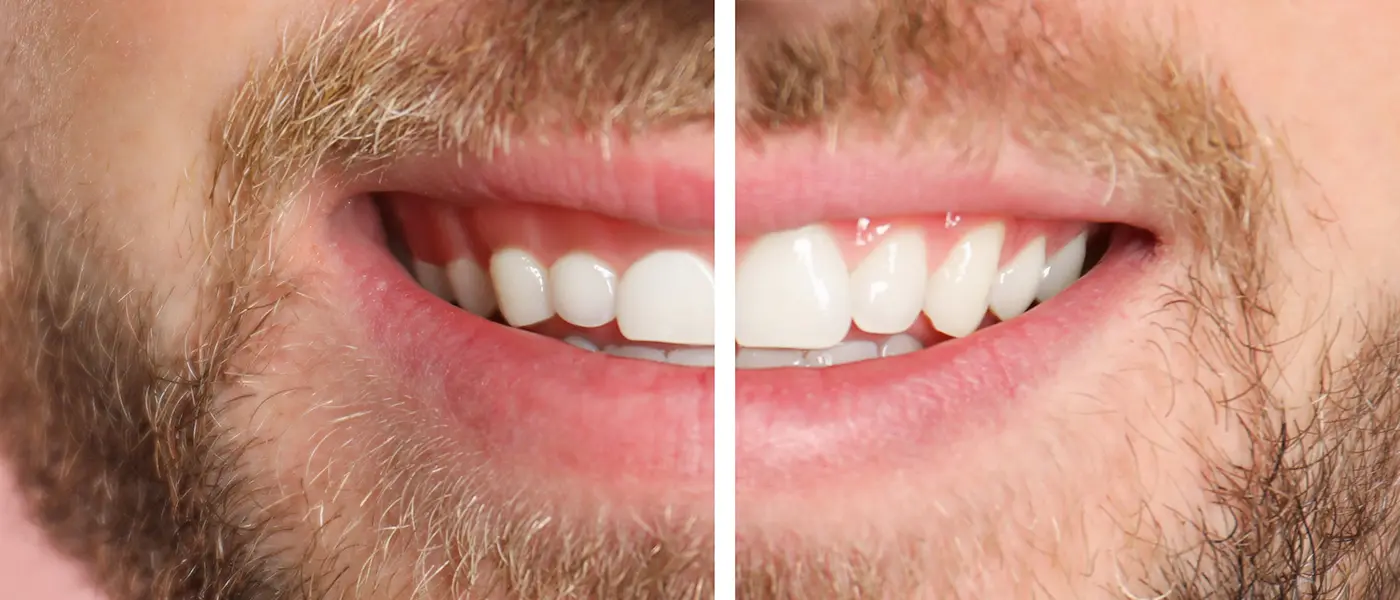
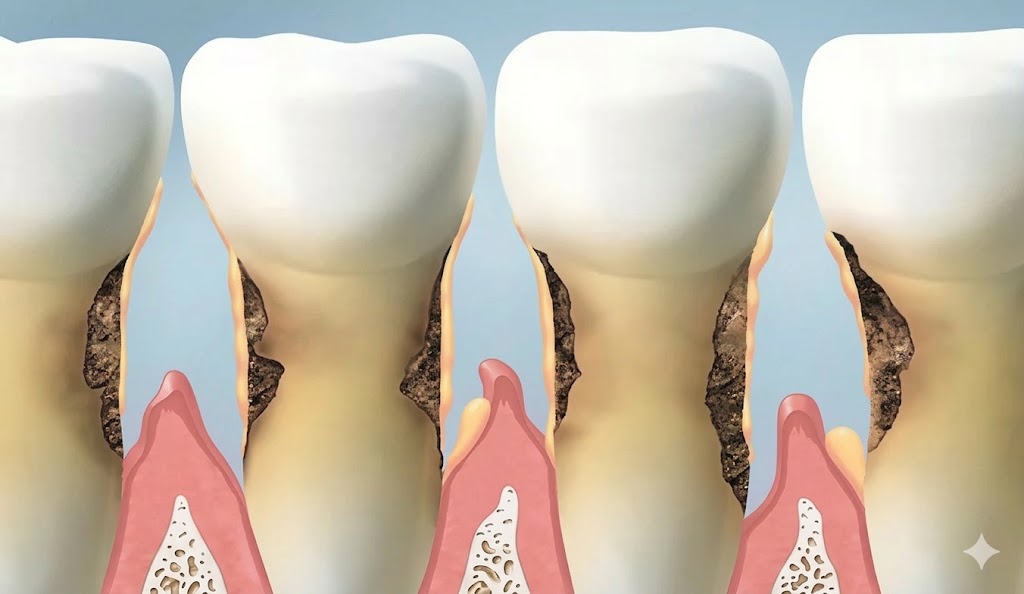
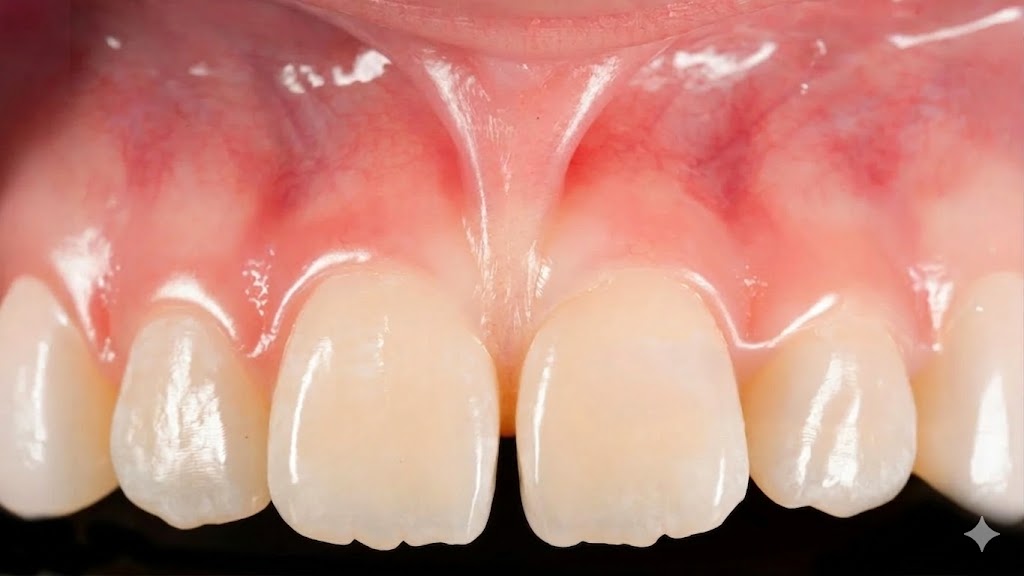
2. Gums That Look Like They're Pulling Away from Your Teeth
If your teeth look longer than they used to, or if you can see the yellowish root surface near the gumline, your gums may be receding. Gum recession is a hallmark sign of periodontal disease — though it can also be caused by aggressive brushing, orthodontic movement, or thin gum tissue.
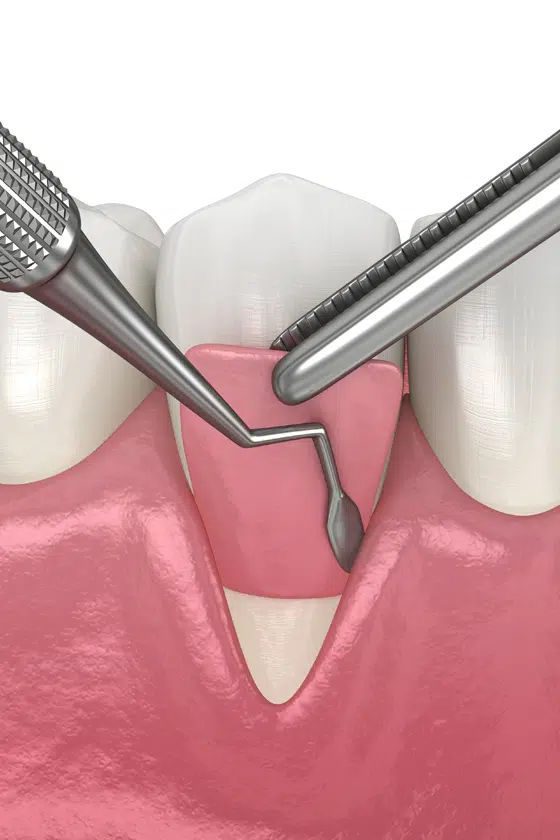
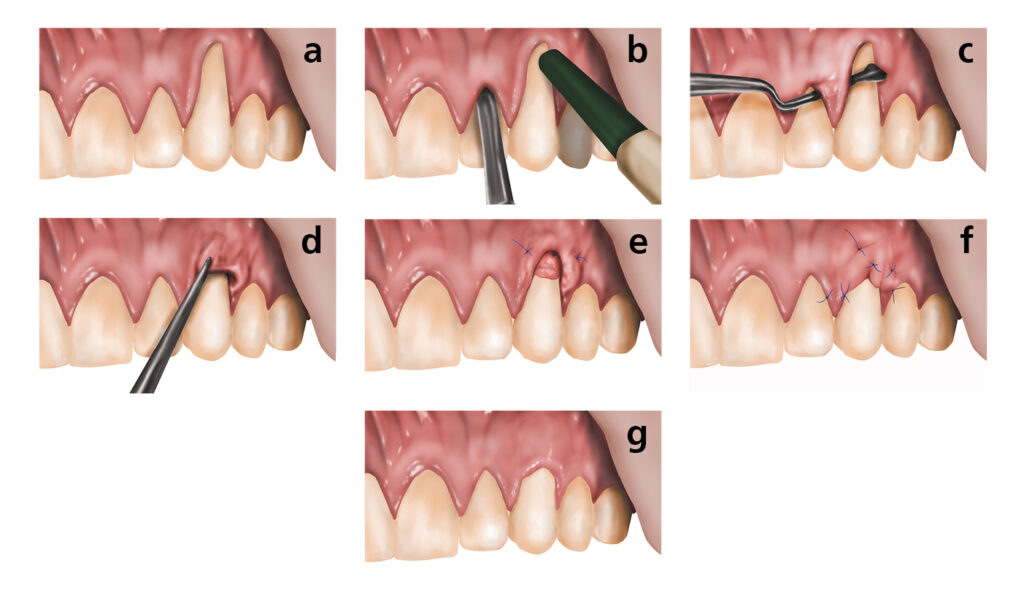
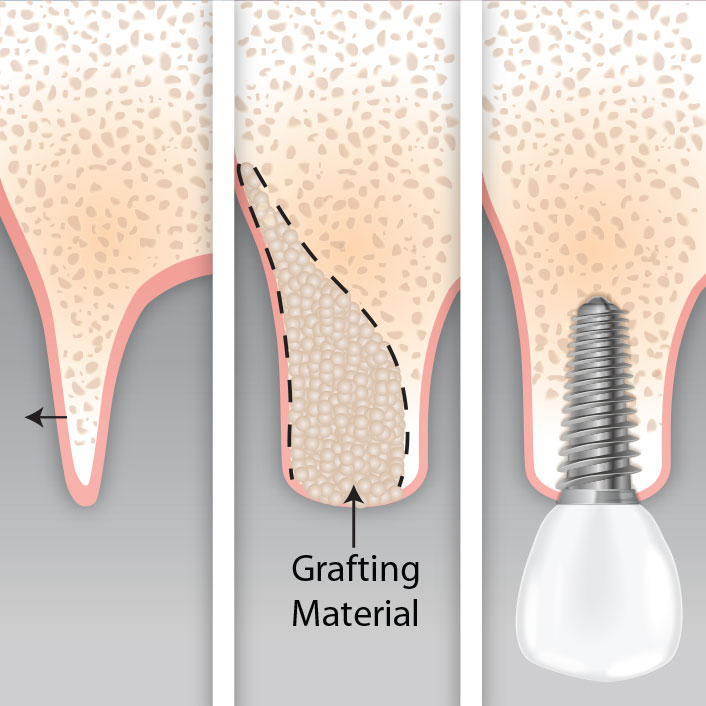
Recession exposes the tooth root, which has no enamel protection. This leads to sensitivity, especially to cold or sweet foods, and significantly increases the risk of root decay. Receded gum tissue does not grow back on its own — but it can be restored with a gum grafting procedure performed by a periodontist.
3. Persistent Bad Breath That Doesn't Respond to Brushing
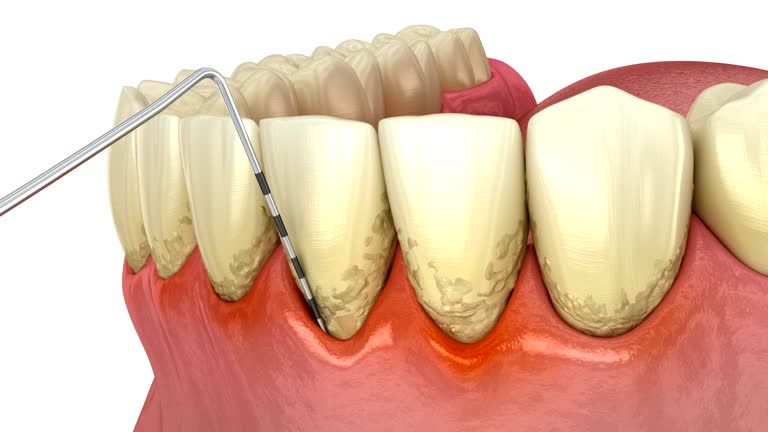
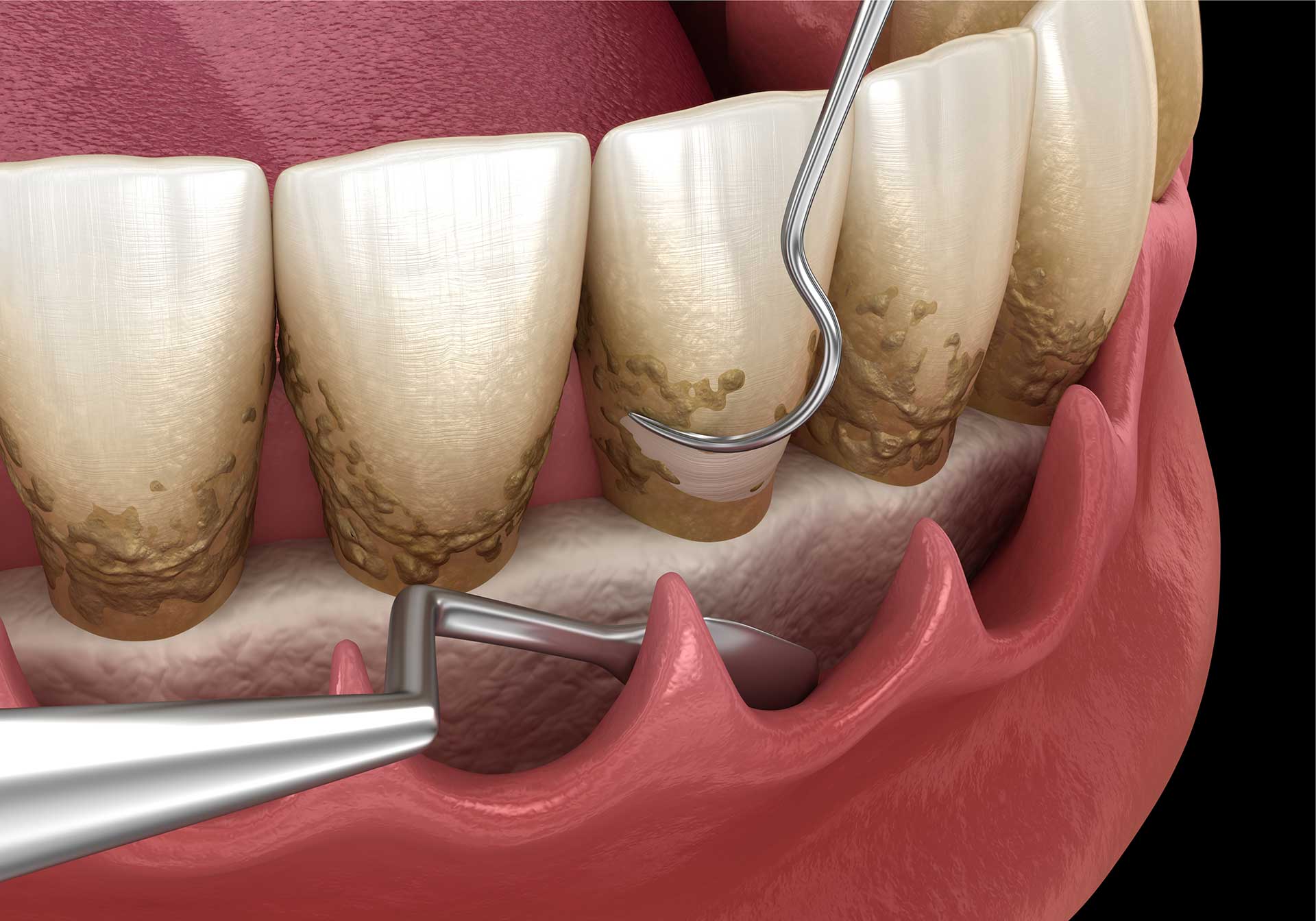
Occasional bad breath is common. Chronic halitosis that persists despite good oral hygiene is different. Bacteria living in deep periodontal pockets — the spaces between your teeth and gums that form as disease progresses — produce sulfur compounds that cause a distinctly unpleasant odor. No amount of mouthwash addresses the source.
If people in your life have mentioned bad breath, or if you notice an unpleasant taste you can't resolve, it's worth getting a periodontal evaluation.
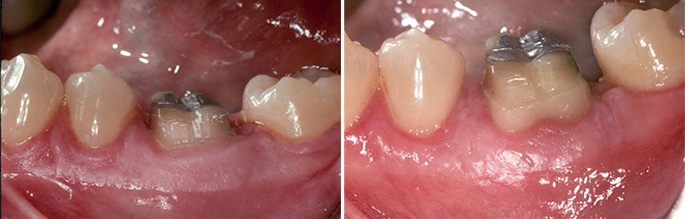
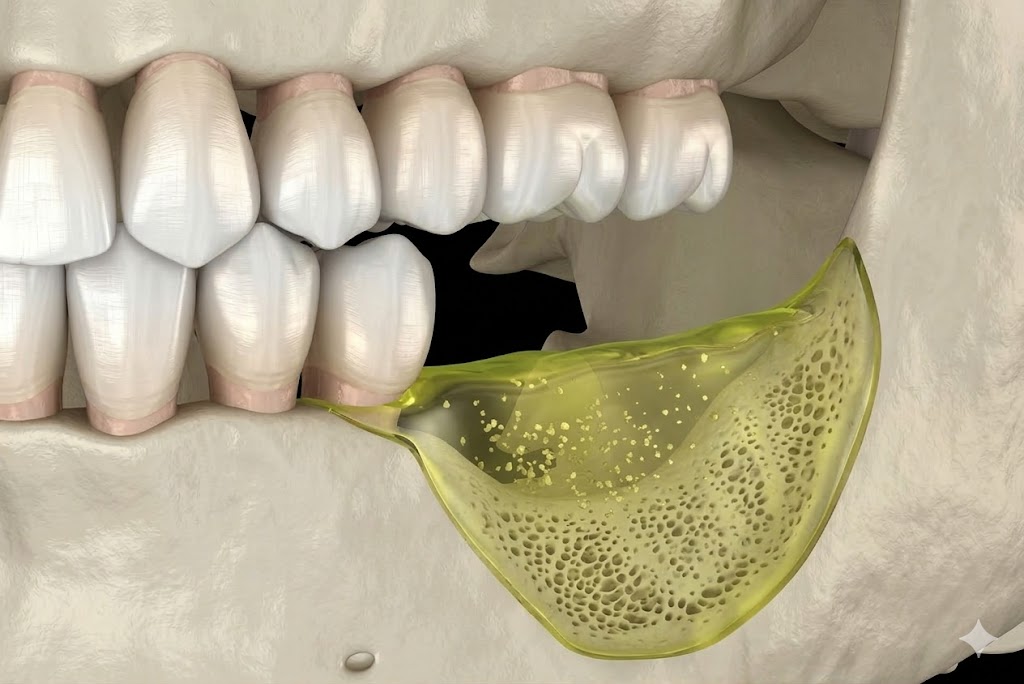
4. Teeth That Feel Loose or Have Shifted Position
Adult teeth should not feel loose. If you notice any mobility — even subtle movement when you press on a tooth — it means the supporting structures (bone and periodontal ligament) have been damaged significantly. Bone loss is the direct cause of tooth mobility in periodontal disease.
Similarly, if your bite has changed, or if teeth that were previously aligned have drifted apart or developed gaps, periodontal disease may be the cause. This degree of progression requires urgent evaluation — the goal is to preserve the remaining bone and prevent tooth loss.
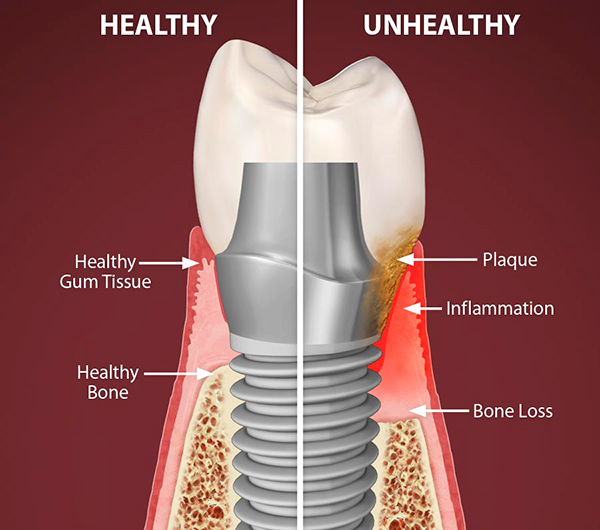
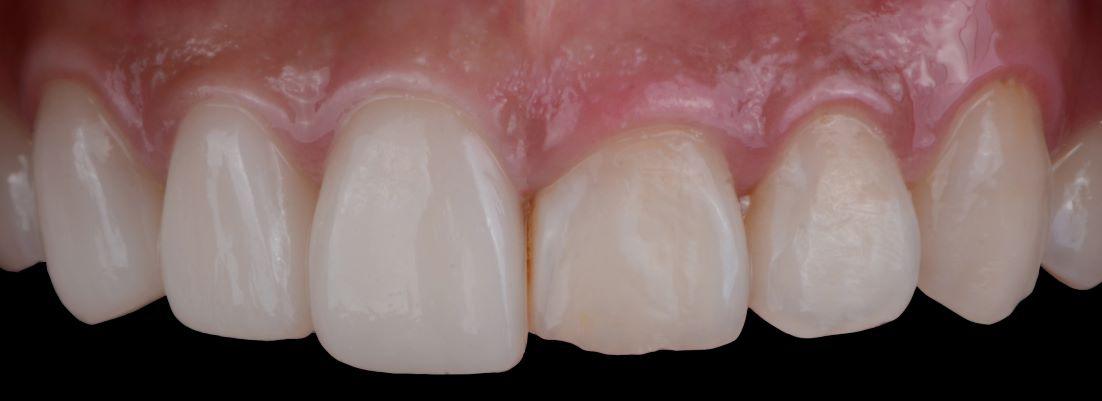
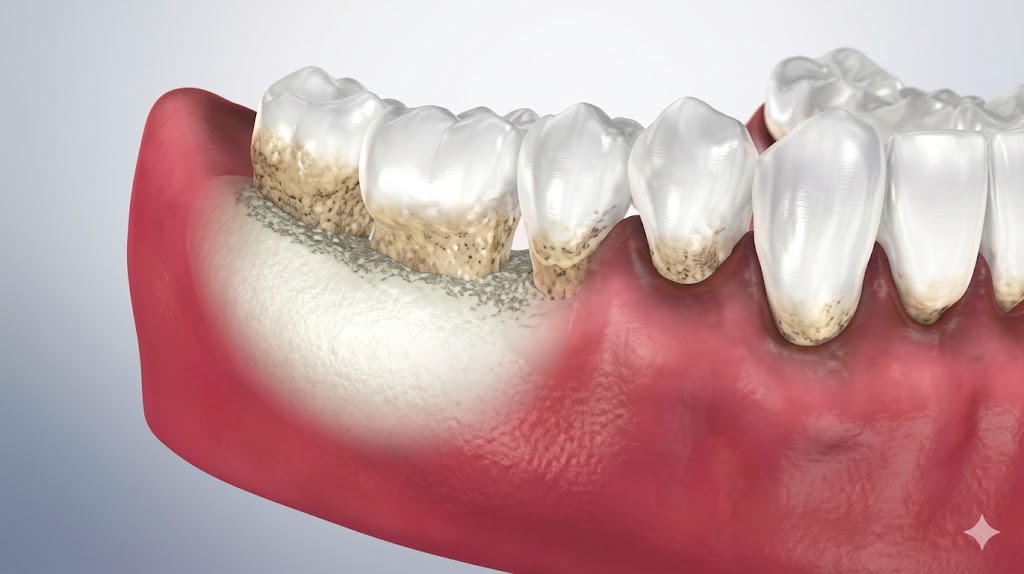
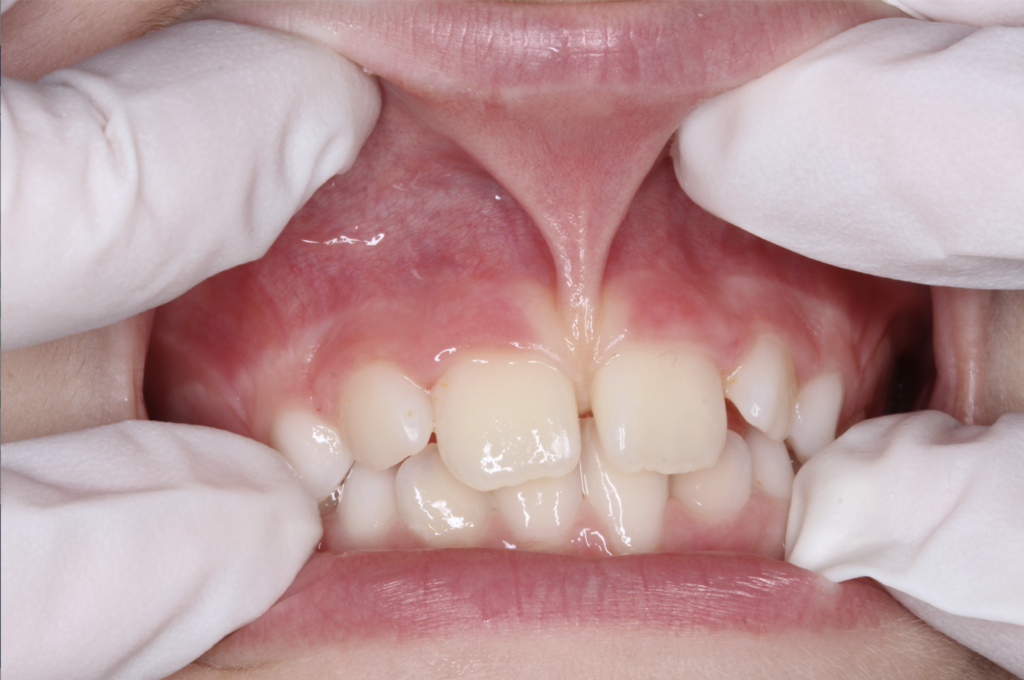
5. Swollen, Red, or Tender Gum Tissue
Healthy gums are firm and pale pink. Gums that are red, puffy, or tender to the touch are inflamed — a response to bacterial infection in the tissue. This can occur around individual teeth or affect the entire gum line.
Some patients notice this most during eating, when gum pressure causes discomfort. Others only notice the discoloration when looking closely in the mirror. Either way, inflamed gum tissue is not cosmetic — it reflects active infection that will progress without treatment.
What to Do If You Notice These Signs
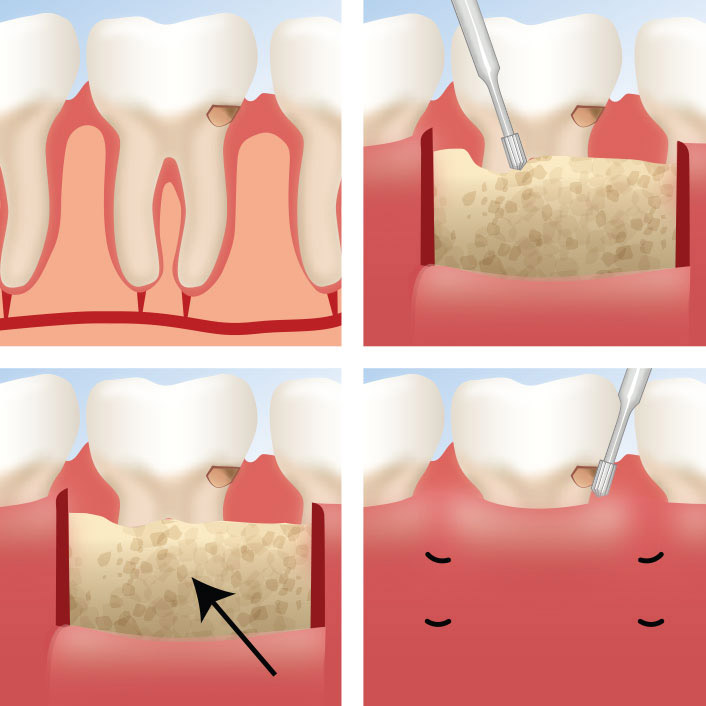
If you're experiencing one or more of the above, the right step is a comprehensive periodontal evaluation. A periodontist is a specialist who focuses exclusively on the health of the structures that support your teeth — bone, gums, and connective tissue. A thorough exam includes pocket depth measurements, bone level assessment via X-rays, and a personalized treatment plan.
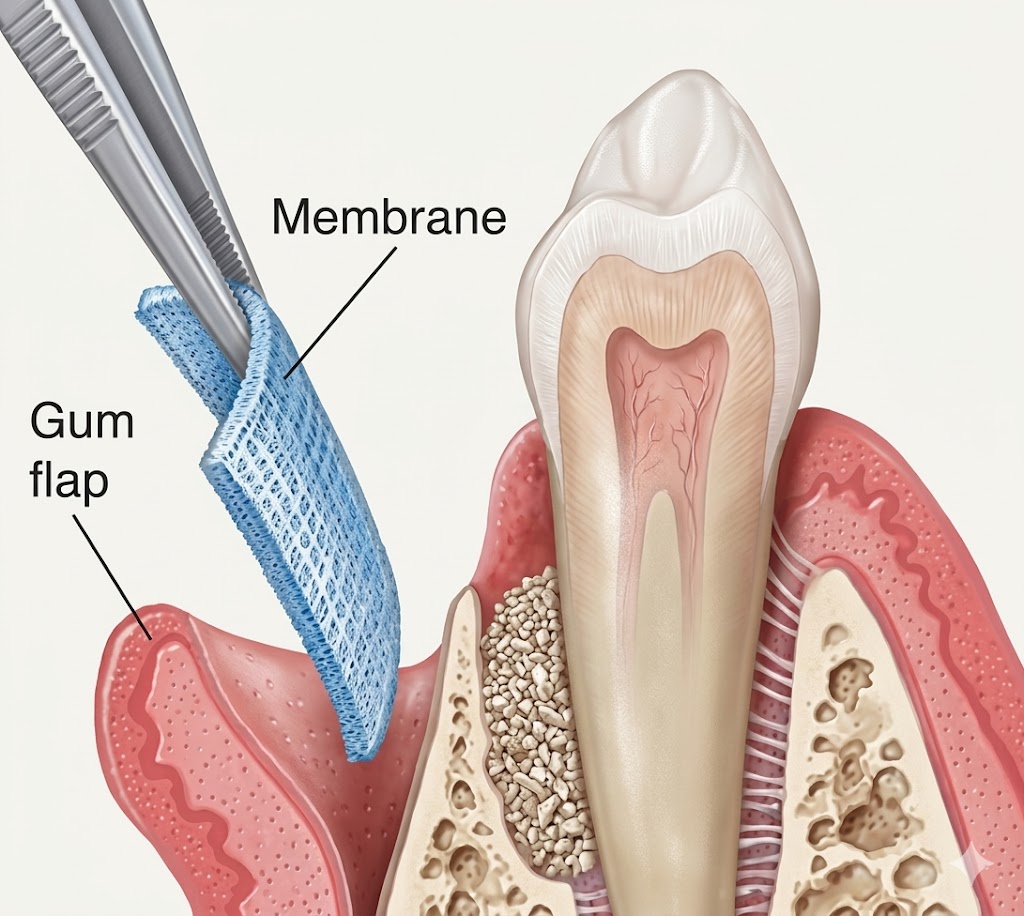
Early-stage gum disease (gingivitis) can often be managed with a professional cleaning and improved home care. More advanced disease may require scaling and root planing, surgical pocket reduction, or regenerative procedures. The sooner you come in, the more options are available — and the more of your natural teeth we can preserve.








%20with%20implant.webp)